Urinary Incontinence – Stress
Urinary incontinence is the loss of voluntary bladder control causing leakage of urine. This temporary or chronic condition has multiple mechanisms and many causes. Each cause has its own methods of diagnosis and its own treatment plan.
Urinary bladder function is a careful balance between pressure from the bladder to empty and resistance from the sphincter (valve) at its outlet. Pressure to empty increases suddenly when the bladder reaches a certain volume.
Sphincter resistance depends not only on the strength of the muscle but also on its position. Both forces are controlled mostly by the autonomic (automatic) nervous system, the same system that regulates body temperature, heart rate, blood pressure, digestion, and everything else the body does without thinking about it. We do, however, have muscle control over the sphincter and can strengthen it with exercise.
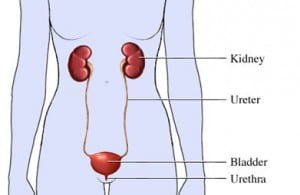

Copyright © Nucleus Medical Media, Inc.
This content was created using EBSCO’s Health Library
Stress incontinence results when certain activities increase pressure on the bladder. Leaking can be triggered by laughing, sneezing, lifting heavy objects, or exercise. This is the most common type of incontinence and may be caused by:
- Weakening of the muscles that support the bladder
- Weakening of the sphincter muscle that controls the flow of urine
This content was created using EBSCO’s Health Library
It is possible to develop chronic urinary incontinence with or without the risk factors listed below. However, the more risk factors you have, the greater your likelihood of developing urinary incontinence. If you have a number of risk factors, ask your doctor what you can do to reduce the risk. Although there are many different causes of incontinence, the risk factors listed here pertain to the most common types of incontinence.
Conditions
The following conditions increase your risk of developing incontinence:
- For women: multiple pregnancies, hysterectomy
- For men: prostate enlargement or prostate surgery
- Dementia
- Overweight and obesity
- Poor mobility
Age
The risk of incontinence generally increases with age.
Gender
Women are more likely to develop stress incontinence.
This content was created using EBSCO’s Health Library
Urinary incontinence may be a symptom of other conditions. Any loss of voluntary bladder control can be considered incontinence. Symptoms include:
- Leaking triggered by laughing, sneezing, lifting heavy objects, or exercise
- A strong urge to urinate followed by loss of urine
- Inability to hold urine long enough to make it to a restroom
- Difficulty initiating urination
- Straining to empty the bladder
- Decreased urinary stream or “dribbling”
This content was created using EBSCO’s Health Library
Urinary incontinence can be a complicated diagnosis because the cause sometimes cannot be fully identified. Your doctor will first ask about the symptoms and medical history, and perform a physical exam. He or she will examine the urinary system and also the nervous system, which controls the bladder function. You will be asked how often you empty your bladder and under what circumstances leakage occurs. A physical exam will look for any physical causes such as blockages or nerve problems. You will be asked to keep a diary of your bladder habits. You may be referred to a urologist or a gynecologist for further evaluation and treatment. Tests may include:
- Urine test —This test will reveal signs of infection and how well the kidneys are functioning.
- Blood test —Although not specific for most causes of urinary incontinence, blood tests reveal much about your general health and help select the most appropriate treatment options.
- Stress test —You will be asked to bear down with a full bladder as your doctor watches for loss of urine. If you are a woman, the doctor will also be looking for the amount of bladder support. The most common cause of stress incontinence in women is relaxation of the floor of the bladder so that it bulges into the vagina when you strain. This bulging changes the angle of the sphincter in relation to the bladder and can cause leakage.
- Ultrasound —An ultrasound device uses high-frequency sound waves to examine structures inside the body. For incontinence, this noninvasive tool assesses structures to determine the amount of urine left in the bladder after voiding.
- Cystoscopy —A cystoscope is a thin tube with a light and a tiny telescope that is inserted into the urethra to view the urethra and bladder. Tumors, narrowing, and other abnormalities can easily be seen. At the same time, x-ray dye can be instilled for x-rays of the bladder and kidneys.
- X-rays —Dye can be introduced into the urinary system either directly through the urethra or indirectly into a vein. Able to reveal many abnormalities, an x-ray taken after you pass the dye will reveal how much residual urine is in the bladder, a sign of obstruction or bladder weakness.
- Urodynamic test —A variety of measurements can be made of bladder function:
- Capacity
- Volume at which the bladder muscle reflexively contracts
- Pressures the bladder muscle generates
- Maximum pressure the sphincter can resist
- Speed of emptying
- Coordination between the sphincter muscle and the bladder muscle
This content was created using EBSCO’s Health Library
Treatments are based on the cause of the urinary incontinence. Physical therapy may be referred as part of a treatment program. Physical therapy programs are designed to correct functional disorders, improve muscle function and strength, relieve pain, promote healing and recovery, and when necessary, help patients adapt to permanent disabilities. Services offered by physical therapists to reduce urinary incontinence may include:
- Comprehensive evaluation
- Myofascial release (internal & external)
- Trigger point release (internal & external)
- Joint mobilization
- Massage
- Patient education
- Heat and ice
- Ultrasound
- Therapeutic exercise for the pelvic floor musculature
- Core strengthening
- Activity modification
- Postural education
- Stretching
- Relaxation techniques
- Biofeedback (internal & external)
- Electrical stimulation (internal & external)
- Muscle re-education
- Bladder and bowel retraining and patterning
- Fluid and food intake management
- Cardiovascular training
- Kegel instruction
This content was created using EBSCO’s Health Library
Urinary incontinence is often a symptom of another condition. It cannot always be prevented but in some cases, incontinence can be managed by:
- Emptying the bladder regularly
- Treating constipation
- Performing exercises to strengthen your pelvic floor muscles, such as Kegel exercises, especially if you are pregnant or have given birth
- Making lifestyle changes, including having a healthy diet (eg, avoiding irritating fluids such as caffeine or alcohol), exercising, losing weight, and quitting smoking
This content was created using EBSCO’s Health Library
This content was created using EBSCO’s Health Library